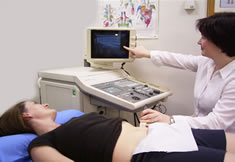
Real Time Ultrasound is a wonderful biofeedback tool where you get to see your deep core muscles work on the screen.
It is vital for all fitness professionals to see and feel how their core muscles are recruited so they are able to teach this to their clients.
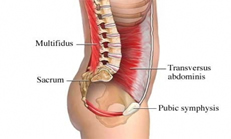
Abdominal muscle cylinder (core) includes the transversus abdominus, pelvic floor muscles, deep lower back muscles (multifidis) and diaphragm. The four parts of the abdominal cylinder work synergistically together to best support the spine. This is referred to lumber pelvic stability in the literature and often spoken of as “neutral” spine.
The deep abdominal muscle transversus abdominus, surrounds the trunk and acts like a natural back brace. The pelvic floor works to regulate bladder and bowel control, support the pelvic organs and is important in sexual function. These muscles work in unison with the diaphragm and other spinal stabilising muscles to provide core stability.
Scientific research has shown that during an episode of low back pain these important deep stabilising muscles, the multifidis, can switch off and waste away long after the pain has settled. They do not automatically return to ideal function on resolution of pain. This is why it is vital after an episode of low back pain that your deep stabilising muscles are assessed. This information should empower fitness professionals that if they are able to teach neutral spine and cue clients correctly recruiting their pelvic floor muscles before exercise they may be reducing recurring episodes of low back pain, stress urinary incontinence and prolapse symptoms.
This information below about Pelvic floor muscle strength training should EMPOWER all Fitness professionals to be comfortable about discussing with clients the pelvic floor muscles and possible associated pelvic floor dysfunctions such as incontinence and prolapse symptoms.
Did you know that
- 65% of women sitting in a GP’s waiting room have some type of incontinence – less than a third will seek your help
- 1 in 3 Australian women suffer from urinary incontinence
- 43% of subjects with incontinence and prolapse depressed their pelvic floor on ultrasound when instructed to lift (straining strategy)
There is :
- Level 1A evidence, Grade A recommendation, Fourth International Consultation on Incontinence (Abrams et al, 2009)
“Pelvic floor muscle training should be offered as first-line therapy to all women with stress, urge or mixed urinary incontinence”
Morphological changes after pelvic floor muscle strength training (RCT):
- Increased muscle thickness, 1.9mm
- Decreased hiatal area by 1.8cm squared
- Shortened muscle length by 6.1mm
- Elevated the position of the bladder by 4.3mm
- Rectum elevated by 6.7mm
- Increase maximal urethra closure by 11.1 mm2.
- Reduced hiatal area and muscle length at maximum Valsalva indicating increased pelvic floor muscle stiffness
- Inhibition of detrusor contraction
Obstetrics & Gynaecology (2010), Hoff Braekken